As Onondaga County schools implement their reopening plans, schools and parents naturally have many questions. The following resources and FAQs should provide a broad range of information. Parents should reach out to their own school district regarding reopening plans or other school-specific information.
School Guidance Documents (OUTDATED):
Frequently Asked Questions: COVID-19 in Schools (OUTDATED)
Q: What guidance is available for school reopening?
Please see the Onondaga County Health Department’s Guidance for K-12 School Reopening, 2021-2022 School Year that was issued on August 13, 2021.
Q: What type of mask should be worn by students and staff during in-person schooling?
Masks, or face coverings, can be used for source control. This means that masks are a physical barrier to help keep respiratory droplets from traveling into the air and onto other people when the person wearing the mask coughs, sneezes, talks, or raises their voice. The following two types can be used in all school settings (in addition to maintaining social distancing whenever possible):
- Medical masks (also called surgical or procedure masks): These are pleated rectangular coverings with elastic ear loops. Compared to the N95 mask, a medical mask filters about 60% to 80% of particles and mostly blocks large-particle droplets, splashes, or sprays that may contain germs. These masks are disposable.
- Homemade fabric masks: The CDC recommends we cover our faces with a scarf or homemade fabric mask in public. The effectiveness of homemade masks varies depending on the fabric used, the style, and the fit. In community studies, homemade masks were found to offer some protection during viral outbreaks. These masks are washable.
PLEASE NOTE that N-95 respirators, masks with exhaust valve, and gaiters are not recommended for routine use by staff and students in schools
Q: Should students and staff wear an N95 mask for in-person schooling?
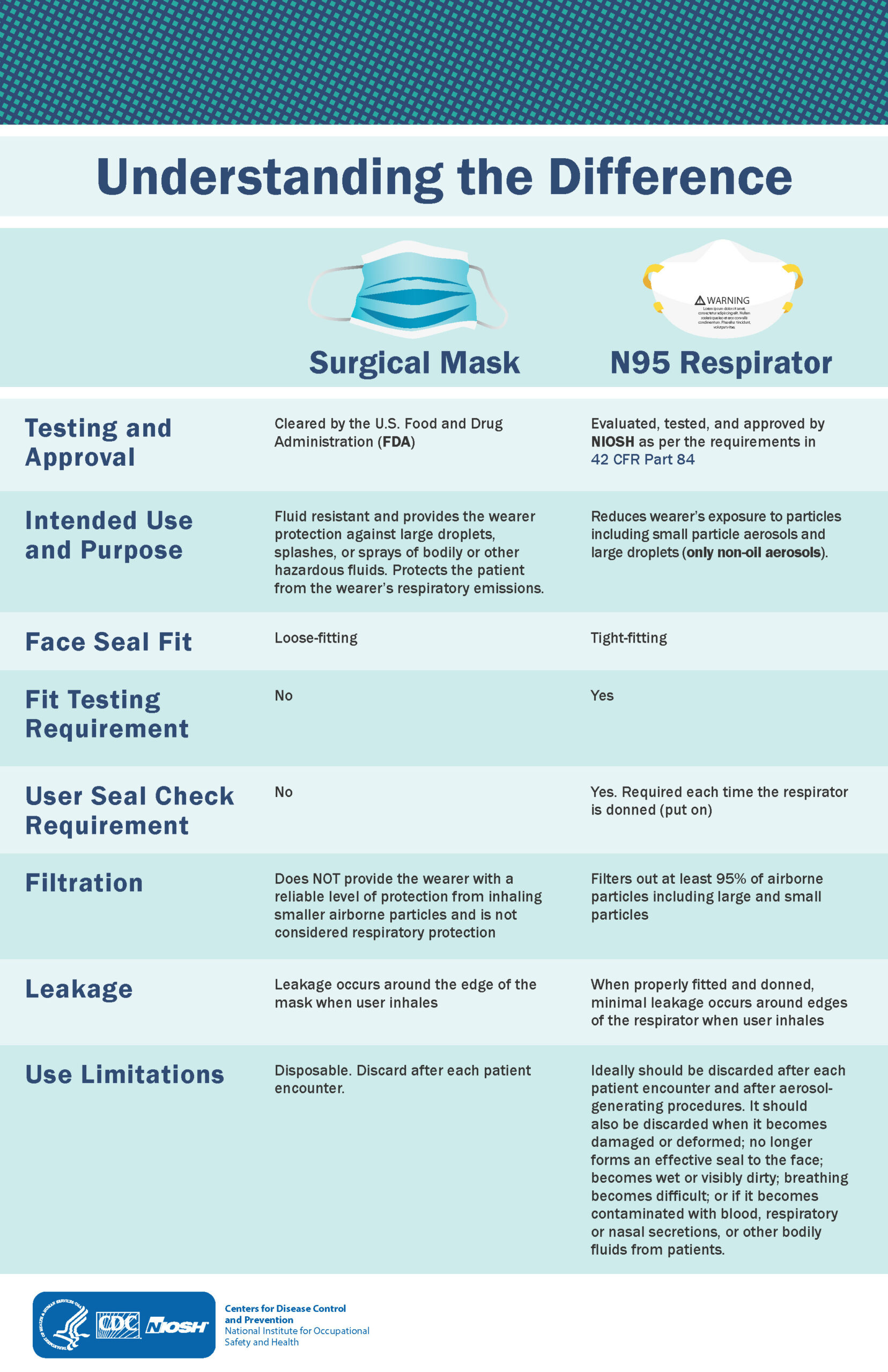
No, N95 respirator masks are designed for medical workers to use during patient care. These masks fit tightly to the face and have the highest filtration efficiency, blocking 95% of particles of 0.3 microns or larger. An N95 mask protects medical workers who come into contact with high doses of the virus while carrying out medical procedures on patients. Medical workers must be fit-tested to a N95 respirator to use it effectively for personal protection. N95 masks are a one-time use product.
See the infographic below to learn more about the difference between N95 respirator masks and medical masks:
Q: How are positive cases handled by the Onondaga County Health Department (OCHD)?
Cases are individuals who have a positive laboratory test for COVID-19. Once the OCHD is notified of a positive case, the individual is contacted and asked a series of questions designed to help us understand how the virus is spreading in our community. Cases are asked to identify anyone they have had close contact with up to 48 hours before becoming sick; or 48 hours from their test date if they are asymptomatic. These contacts will be followed up with by contact tracers. Based on the investigation, the OCHD will place a case under isolation for 10 days from the date they started feeling sick, or 10 days from the date of their test if they are asymptomatic. Each case will receive an official isolation order.
Q: When and how should the school report positive COVID-19 cases to the Onondaga County Health Department (OCHD)?
If the school is notified first (before OCHD) of a student’s or staff member’s positive test result, immediately notify the OCHD by calling 315.435.3155. Our business hours are Monday–Friday 8:30 am – 4:30 pm. After hours, please send any positive COVID-19 cases to our secure fax at 315.435.3884. Case investigations and contact tracing work continue over the weekend.
Q: Who is responsible for contact tracing for students, faculty, and staff?
As with case investigation, the OCHD has primary responsibility for contact tracing; however, effective contact tracing in the school environment is a collaborative effort between the school and the OCHD. The health department will need the assistance of schools to provide staff and student rosters, schedules, and other information to identify exposed individuals, arrange for testing, etc. The contact tracer will also identify people outside of the school setting who may have been exposed to the case, and complete the appropriate follow-up.
Q: Will contact tracers release the name of the positive individual to their contacts?
No. Contact tracers will tell potentially infected persons that they were exposed and they will not disclose the identity of the person to whom they were exposed. In some situations, the positive case has already reached out to their contacts and notified them of their positive status.
Q: How long will contacts of positive COVID-19 cases be required to quarantine?
Individuals who are exposed to someone with COVID-19 will be required to quarantine for 10 days from the date they were last exposed. Fully vaccinated people who have been exposed do NOT have to quarantine unless they have symptoms (see this flowchart for details). Those who are placed in quarantine will receive an official quarantine order. After stopping quarantine, individuals should:
- Watch for symptoms until 14 days after exposure.
- If symptoms develop, immediately self-isolate and contact the Health Department at 315.435.3236.
- Wear a mask, stay at least 6 feet from others, wash hands, avoid crowds, and take other steps to prevent the spread of COVID-19.
Q: If a contact is tested during the 10 day quarantine period and is found to be negative, does the quarantine end early?
Contacts must remain in quarantine for the full duration listed on the initial quarantine order in case symptoms develop. They cannot “test out” early.
Q: What resources will a person in isolation or quarantine require?
A person in isolation or quarantine will need access to a private room and a private bathroom. If a private bathroom is not available, cleaning and disinfecting must be done after each use. Individuals will also need access to food, medications and other essential items (such as access to remote instruction) that will allow them to remain in isolation or quarantine. People who need assistance during quarantine or isolation can call the OCHD at 315.435.3280.
Q: Where can students, faculty and staff get tested for COVID-19?
A list of testing sites can be found here. Students, faculty, and staff can also call the NYS COVID-19 hotline at 1.888.364.3065 for assistance locating a testing site, or contact their primary care providers.
Q: Is there a charge for COVID-19 tests conducted at state-run facilities?
No, there is no out-of-pocket charge for COVID-19 tests conducted at Onondaga County or state-run facilities, though insurance information may be requested. For other testing sites, please check with the site or your insurance provider to confirm any costs that may be associated with the test. You may also contact your primary care provider to ask about testing.
Q: When can a person who has tested positive for COVID-19 return to school?
If a student or staff member tests positive for COVID-19 the release from isolation protocol is as follows:
If an individual is experiencing symptoms (fever, cough, shortness of breath/difficulty breathing, chills, repeated shaking with chills, muscle pain, headache, sore throat, or new loss of taste or smell), the following criteria must be met before they can be released from isolation:
- It’s been at least 10 days since the person first started experiencing symptoms; AND
- The person hasn’t had a fever in at least 3 days without taking a fever-reducing medication (such as Tylenol); AND
- Symptoms associated with COVID-19 have improved.
If an individual has not experienced symptoms, the following criteria must be met before they can be released from isolation:
- It’s been at least 10 days since the person’s first positive COVID-19 test was collected, AND
- The individual hasn’t had any subsequent illness
Q: Can we assume that students with antibodies are safe from contracting COVID-19?
We currently do not have enough information about the significance of antibody tests. Antibody tests also CANNOT diagnose if an individual has active infectious COVID-19.
Q: Are rapid COVID-19 tests (Antigen or Molecular) reliable?
Rapid tests are useful because they provide results in under an hour. The test result must be interpreted in the context of clinical signs and symptoms. For more information please visit https://www.cdc.gov/coronavirus/2019-ncov/lab/resources/antigen-tests-guidelines.html
Q: Why is the positive case my child was exposed to being released before my child is released from quarantine?
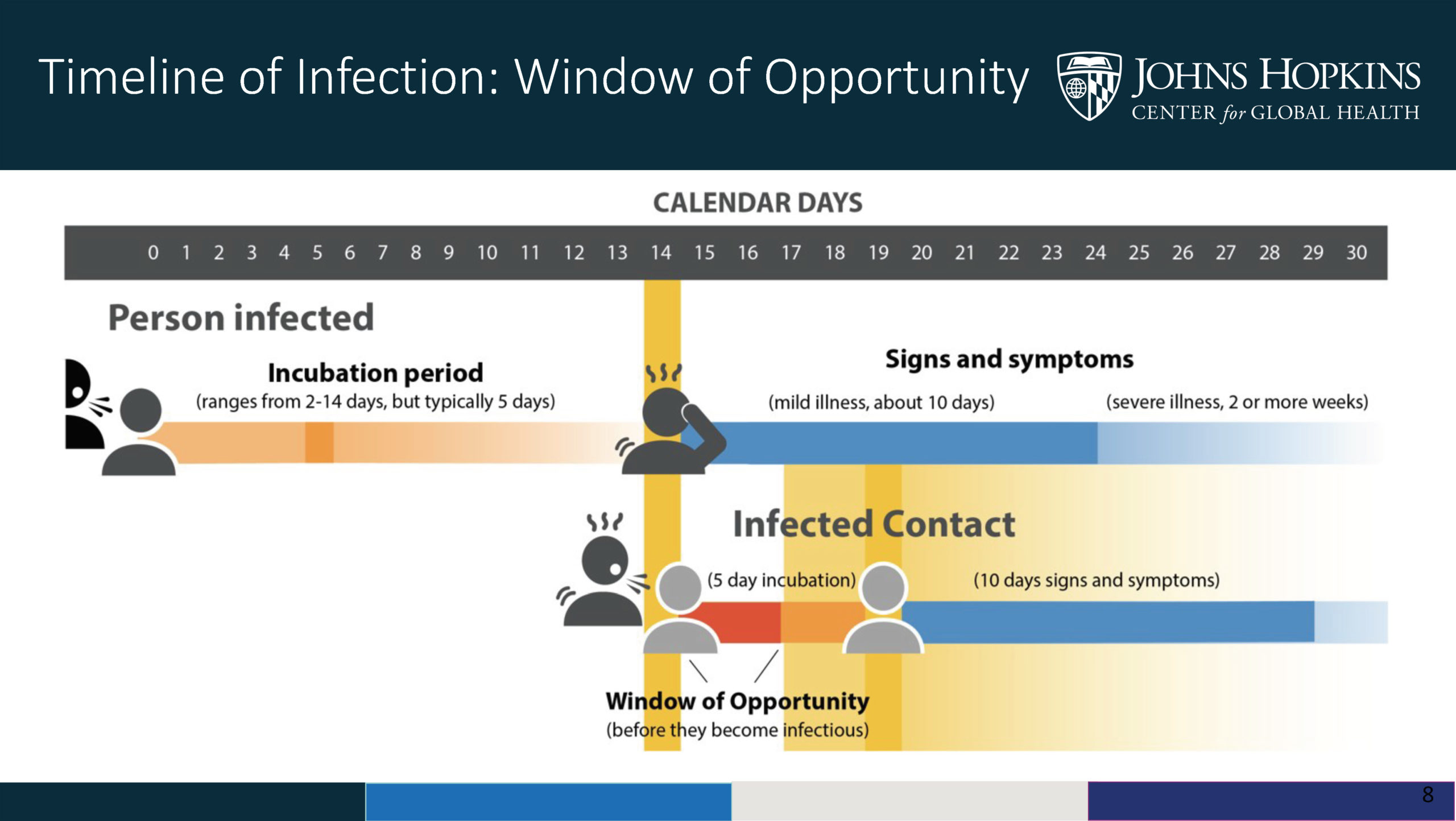
When a person is exposed to COVID-19, it can take time for the person to develop the disease (incubation period). This is why the quarantine period may continue past the release date of the positive case.
Q: Can you leave quarantine to get a COVID-19 test or does your quarantine start all over after you went out to get that test?
Yes, you can leave quarantine to get a COVID-19 swab test. However, during travel to and from testing, you should not make any other stops, be sure to wear a mask/face covering, observe distancing, and utilize private means for transportation. While your quarantine period does not re-start, you must continue to quarantine for the full 10 days from the last exposure to a COVID-19 positive individual, even if your test is negative.
Q: In the event there is a large exposure, what is the plan if OCHD gets overwhelmed with the caseload once school starts?
The OCHD has been working in conjunction with the New York State Department of Health on contact tracing, using a joint system for tracking cases and contacts. This system allows for increased capacity of contact tracing.
Q: If a child tests positive and has a sibling in the school, should the school keep the sibling out of school?
Yes, unless the siblings reside in separate households, the sibling must be placed on quarantine which would mean that the sibling should not attend school during the required period for quarantine.
Q: If a student/staff member is home on quarantine and then develops symptoms, please explain how that impacts attendance to school/work and what it means for the siblings that may have been continuing to go to school?
Students or staff who are home on quarantine and develop symptoms should get tested. If a student or staff tests positive, their household members will likely be considered close contacts and will need to be quarantined. The individual testing positive will require isolation for 10 days.
Q: If someone has to quarantine and has a family member in isolation, would they be released on the same day?
The quarantine period is 10 days from the last date of contact with an individual who is positive for COVID-19. Therefore the release dates are usually different.
Q: If a person travels internationally, but their child who lives with them did not travel, does the child also have to quarantine, or can they attend school?
The child may attend school as long as the traveler in the household remains asymptomatic and does not test positive for COVID-19.
Q: Does the student have to quarantine if the parent had contact and is quarantining, but does not have symptoms?
If a member of the household is quarantining because of either a known exposure to a COVID-19 positive individual or because of traveling, other members of the household can leave the home if that person can quarantine properly from the household members. A quarantined person should:
- Separate themselves from other members of the household
- Use a separate bedroom and bathroom
- Do not share linens, towels, eating utensils, cups, and plates
- Limit time in common household areas, such as kitchens
Q: What is the timeframe for contract tracing? Will you work with the school immediately? What if we are notified in the evening and siblings may be at school in the morning?
Local health departments aim to contact positive individuals within 24 hours of receiving a positive lab report. Schools should be conducting daily health screenings, including asking whether the child/staff has been in contact with a person who has tested positive.
Q: Do schools need parental permission to send COVID-19 related medical information to OCHD?
COVID-19 is a reportable communicable disease mandated under the New York State Sanitary Code (10NYCRR 2.10, 2.14), including reporting by school nurses (10NYCRR 2.12). See https://regs.health.ny.gov/volume-title-10/content/reporting-cases-records and https://www.health.ny.gov/forms/instructions/doh-389_instructions.pdf.
Q: Is there a threshold of infections or absentee rates that would indicate a school should close?
The OCHD does not make the decision as to whether a school or classroom should be closed because of COVID-19. The OCHD may be consulted on a case-by-case basis, but the decision rests solely with the school and school district. The Onondaga County Commissioner of Health has the legal authority to determine who needs to isolate and quarantine due to COVID-19 positive cases and/or exposure to a COVID-19 case.
Q: What parameters/conditions/metrics should we use as an early warning sign that positive cases or absenteeism are increasing beyond an acceptable rate?
Generally, schools can remain open if the daily infection rate remains below 5% using a 14-day average. Schools will close if the regional infection rate rises over 9%.
Q: In regards to screening, should it be prior to entering the building or before they leave their house?
School districts are required to have a protocol in place to perform temperature and health screenings for COVID symptoms. Screenings by the parent/guardian prior to school are preferred. Symptomatic individuals should not leave their households. Parents/ guardians/ students should be provided with information explaining the importance of monitoring for symptoms and remaining at home whenever symptoms are recognized. Please see the New York State Education Department’s (NYSED) Reopening Guidance for more information.
Q: Previously, if there was a case, we had to close a building for 24 hours. Is that still the case?
A single case of COVID-19 in a school would not warrant closing the school. Additional cleaning using EPA-approved products should be focused on the locations where the case was, and the objects handled by the case.
Adapted from the Westchester County Health Department │ August 2020